PrescriptSure · Pitch Deck
Seed · 2026
Verify coverage before the prescription becomes a problem.
PrescriptSure helps clinics verify prescription coverage before the script is sent — cutting delays, rework, and patient drop-off.
Presented By
Shady Kassoumeh
Founder & CEO
Contact
sk@prescriptsure.com
Web
www.prescriptsure.com
The Problem
Every prescription starts with a list of questions nobody can answer fast enough.
At the point of prescribing
- 01Is this drug covered under this patient's plan?
- 02Will prior authorization be required?
- 03Is step therapy going to block this prescription?
- 04What clinical criteria are needed for approval?
- 05Is there a covered alternative that avoids the delay?
Market Pain Points
The Impact
The damage shows up across admin staff, physicians, and patients.
Admin Staff
- Time lost to payer portals, formularies, and coverage calls
- More rework, callbacks, and wasted staff effort
- No clear view into whether a prescription will actually go through
Physicians
- Less time for patient care
- More guesswork in prescribing
- PA, step therapy, and criteria barriers discovered too late
Patients
- More delays and coverage surprises
- Higher risk of abandonment at the pharmacy
- Less confidence in the treatment plan
Our Solution
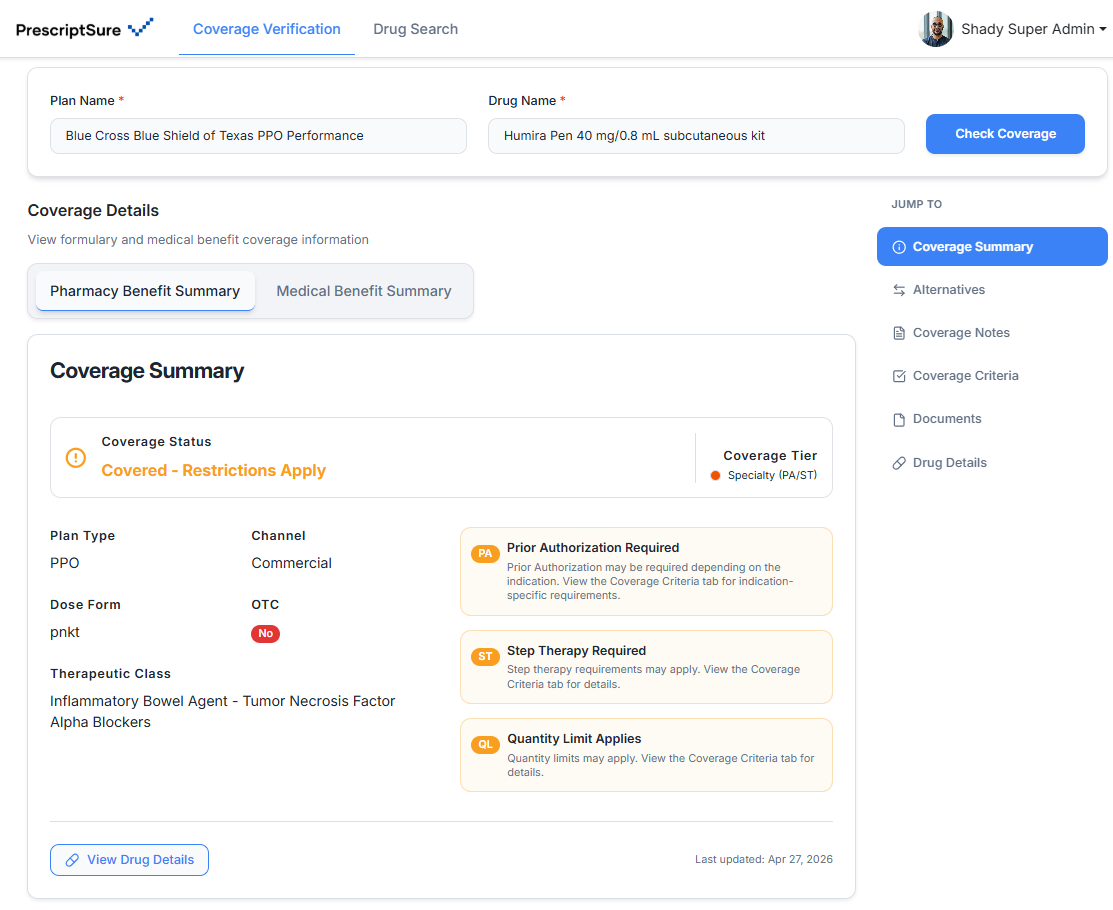
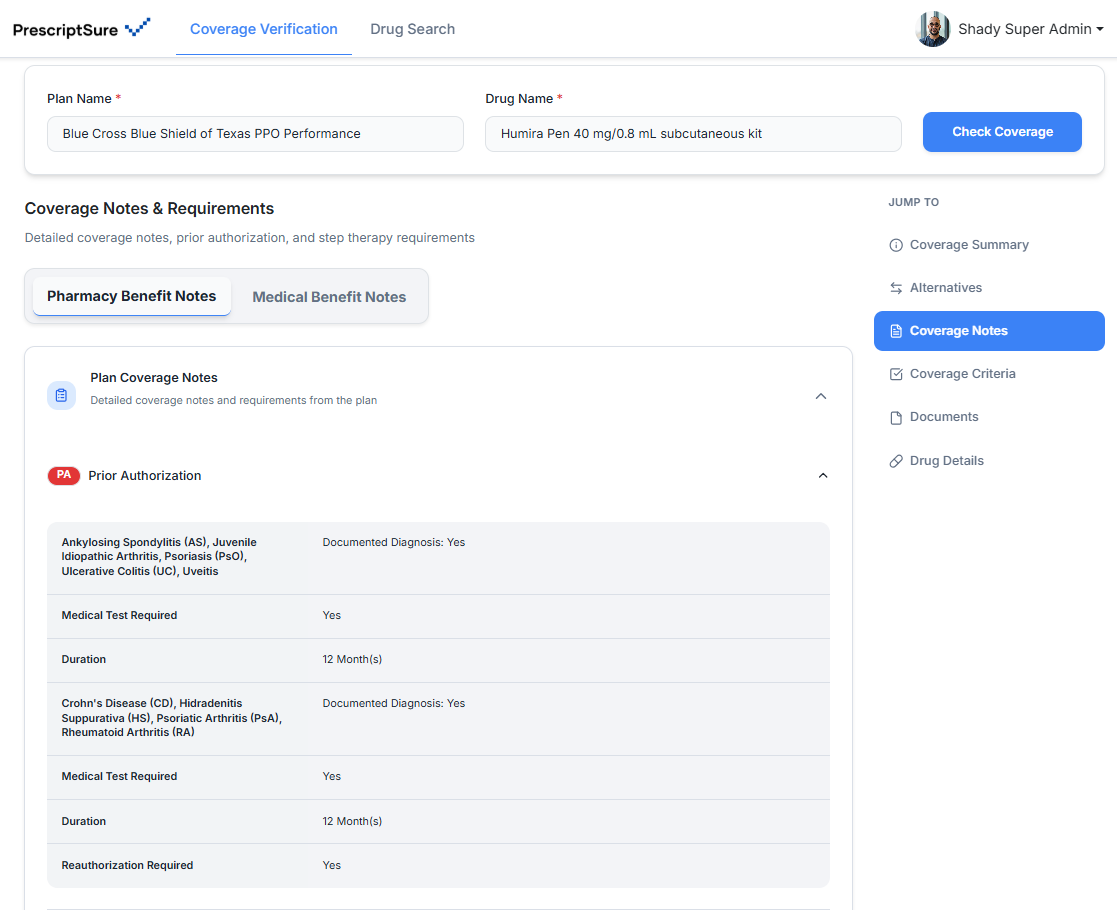
The coverage verification layer for modern prescribing.
PrescriptSure helps clinics verify coverage before the prescription is sent — so providers know what is covered, what is required, and what is most likely to get through.
Why It Matters
Clinicians
- Faster prescribing decisions
- Fewer coverage surprises
- Less manual research
Administrators
- Lower administrative waste
- Better staff efficiency
- Fewer lost prescriptions
Patients
- Fewer delays
- Fewer pharmacy surprises
- Better access to treatment
Workflow Today vs. PrescriptSure
From manual research to workflow-native coverage intelligence.
Today, specialists spend too much time jumping across payer portals, formularies, and criteria sources. PrescriptSure compresses that work into one workflow — so teams can validate, submit, and move faster.
Today
8 stepsDominated by manual research
- 01Order submitted
- 02Check for PABottleneck
- 03Manual payer lookupBottleneck
- 04Research formulary and criteriaBottleneck
- 05Draft justification
- 06Submit and follow up
- 07Track status
- 08Authorization obtained
With PrescriptSure
6 stepsResearch is streamlined
- 01Order submitted
- 02PA requirements and criteria surfaced
- 03Specialist validates instead of researches
- 04Draft justification from structured data
- 05Submit to payer
- 06Authorization obtained faster
Why Now
Five forces are converging to make prescription access intelligence a must-have layer.
Regulatory
CMS is accelerating electronic prior authorization modernization, pushing payers and platforms toward faster, more standardized workflows.
Drug Mix & Volume
GLP-1s, oncology drugs, biologics, and other specialty medications are increasing pharmacy PA volume, cost, and complexity.
Market Demand
Clinical software is moving faster, but prescription access remains a major bottleneck in the prescribing workflow.
Technology
New infrastructure standards now make real-time prescription intelligence usable at scale inside clinical workflows.
Structural Pressure
PBM reform and broader transparency pressure are making medication access intelligence more important for payers, platforms, and care delivery organizations.
Competitive Landscape · Why We Win
PrescriptSure brings coverage verification, criteria, and workflow together at the prescribing moment — in a way existing tools do not.
Compared to Alternatives
Why We Win
Right Moment
We sit before delay, denial, and rework begin.
Stronger With Usage
Coverage logic and workflow intelligence compound over time.
Scales Through Workflow
EHR and partner integrations increase stickiness and make us harder to replace.
Market Opportunity
A focused wedge into a large and expanding prescription access market.
Entry Market
Prescription coverage verification for ambulatory and SMB clinics, where the problem is urgent, frequent, and expensive enough to drive near-term adoption.
Expansion Market
EHR-integrated prescribing, prior authorization, and medication access workflows — where embedding into clinical workflow expands distribution, increases product stickiness, and creates stronger monetization opportunities.
Long-Term Platform Opportunity
Prescription access intelligence delivered through software, APIs, and embedded workflow infrastructure across providers, platforms, and partners.
Business Model
Start with software revenue, then expand into higher-leverage monetization.
SaaS Subscriptions
Per-seat monthly and annual pricing for clinics and ambulatory groups, with premium modules over time.
Enterprise / Platform Licensing
Annual licensing for EHRs, health IT platforms, and workflow partners that embed PrescriptSure into clinical workflows.
Data / API Monetization
Over time, PrescriptSure can expand into API licensing and data-driven intelligence products as usage, integrations, and proprietary workflow data scale.
Traction
We are not only modeling this. We are measuring it.
Measured Today
First Channel Partner
athenahealth
180K+
Providers
10K+
Clinics, facilities & orgs
- 01Approved for direct API integration
- 02NDA, contract, and developer access in place
- 03Integration path underway
Early Investor Commitments
3
Private investors committed
$125K
Total investor commitments
Go-to-Market
Win SMB clinics first, then scale through EHR channel partnerships.
Motion
Initial Beachhead
Small to medium-sized clinics are our entry market — where the pain is urgent, the workflow is frequent, and the path to adoption is direct.
Direct Clinic Motion
Drive early traction through direct outreach to SMB clinics, focusing on medical assistants, office staff, and prescribing workflows most affected by prescription coverage friction.
Channel Expansion (EHRs)
Expand into mid-tier EHR vendors as a core growth channel. Our goal is to become the coverage verification layer inside their platforms and improve how they solve this problem today.
AAMA Distribution
Use the AAMA network as a targeted outreach channel through access to a 70,000-member medical assistant mailing list.
Execution Goals
- 01Prove product-market fit with SMB clinics
- 02Win early traction through direct adoption
- 03Establish the first EHR channel partner
- 04Expand distribution through additional EHR vendors
The Ask
Raising $750,000 to prove product-market fit by reaching 100 active clinics and launching our first EHR integration.
Raise
$750,000
Structure
SAFE
Post-Money Cap
$5M
Discount
20%
Runway
12 months
Use of Funds
What This Funds
- 01100 active clinics
- 02athenahealth integration live
- 03Clear product-market fit signals in the SMB clinic segment
- 04Validated path to repeatable EHR channel partnerships
The Team
Founding team and advisor.

Shady Kassoumeh
Founder & CEO
GTM strategy, customer development, product direction, and fundraising.

Mohmmad El-zaghah
Co-founder & CTO
Healthcare-grade cloud architecture, product engineering, and EHR integration execution.

Leen Habbal
Co-founder, Product & UX
Workflow design, product adoption, and clinician-centered user experience.

Dr. Samer Nachawati, DO
Co-founder, Clinical SME
Real-world prescribing and PA workflow insight from frontline clinical practice.

Larry Warnock
Advisor, Venture & GTM
Enterprise GTM, investor strategy, and strategic market access.
Why This Team Can Win
- 01Built for healthcare-grade infrastructure and workflow integration
- 02Grounded in real clinical prescribing and PA pain
- 03Designed for adoption inside high-friction healthcare workflows
- 04Positioned to execute both direct GTM and EHR channel expansion

PrescriptSure is building the coverage verification layer for modern prescribing.
Our goal is to become the de facto solution for prescription coverage verification across SMB clinics and mid-tier EHRs.
Why We Believe This Matters
- 01The problem is painful, frequent, and expensive
- 02The workflow value is immediate
- 03Early traction and measured workflow data support the opportunity
- 04athenahealth gives us a credible first channel path
- 05The wedge is clear, with meaningful expansion potential
The Ask
$750,000
To accelerate product-market fit, activate 100 clinics, launch the athenahealth integration, and establish a repeatable EHR channel model.
Thank you.
Shady Kassoumeh
Founder & CEO
sk@prescriptsure.com
www.prescriptsure.com